What Life Is Like After Being Taken Off a Ventilator
A near-death experience in the ICU could have lasting effects on the brain—from PTSD to cognitive impairment on par with mild dementia.
/media/video/upload/Ventilator_Single_04_Red-1_YSwPbuZ.mp4)
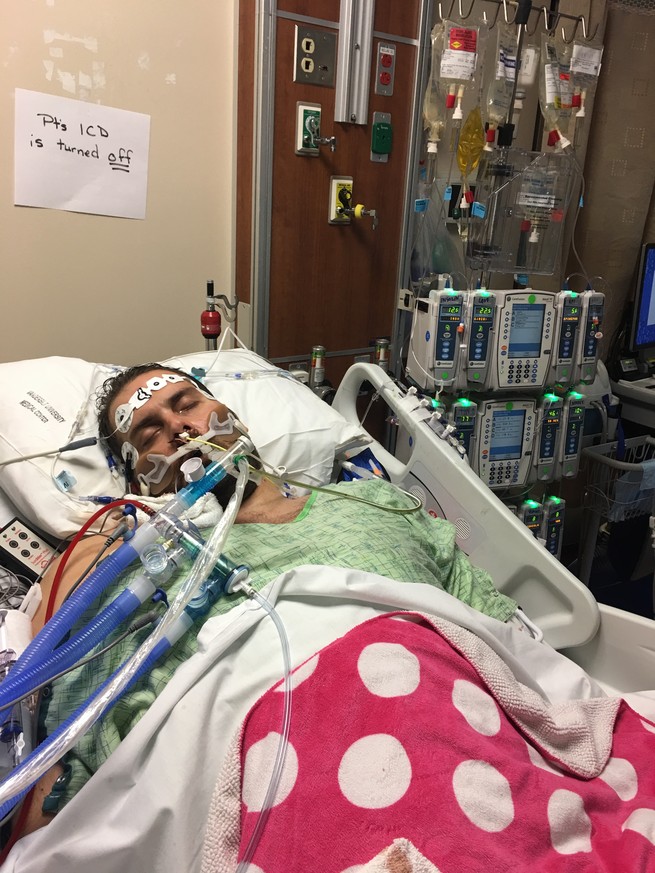
Even after Kyle Mullicane came home from the ICU, he would have nightmares about being back in the hospital, struggling to breathe. He had been on a ventilator, but his body fought so hard against the breathing tube in his throat that his arms and legs had to be restrained. Immobilized, he tried to chew through the plastic. In his post-ICU dreams, he would succeed at doing so, only to suffocate as the broken pieces fell into his lungs.
It has been eight months since Mullicane, 35, survived multiple organ failure from a bad reaction to heart medications. Physically, he feels well enough to have hiked a national park in January. But mentally, he’s still recovering. “My memory is shot,” he says. Loud noises startle him. And while the nightmares have gotten better, he remembers vivid hallucinations from the ICU, when doctors and nurses appeared to him as witches with shimmering faces. Even at home, normal life doesn’t quite feel normal. “I don’t feel safe anymore,” he says, “like there’s a low hum of menace.”
In hospitals across America, thousands of the sickest COVID-19 patients are now needing intensive care. The marvels of 21st-century medicine will help keep them alive in the best-case scenarios. But surviving can be just the start of a long recovery, and even after this pandemic fades, some survivors might have to face lingering aftereffects. For reasons still not entirely understood, some patients may develop what’s known as “post-intensive-care syndrome,” which can include a constellation of physical, cognitive, and psychological symptoms. About 1 in 10 of all patients who have been in the ICU have PTSD. About 30 percent experience depression. Thirty percent have symptoms of anxiety. And another 40 percent report cognitive impairment on par with moderate brain injury.
“It isn’t intuitive that being in the ICU for a lung condition would have an obvious consequence for your brain,” says James Jackson, the director of long-term outcomes at Vanderbilt University’s ICU Recovery Center. But the combination of a near-death experience, sedation, and a phenomenon called “ICU delirium”—likely exacerbated by sedative drugs—can have lasting effects.
Sedation is necessary for many patients in the ICU, especially ones with COVID-19, as part of being on a ventilator. This requires threading a plastic breathing tube down the throat and past the vocal cords into the upper chest, which conscious patients will instinctively fight. “Put it this way: If you have a tube down your throat and it doesn’t bother you, there’s something wrong,” says John Kress, a pulmonary and critical-care doctor at the University of Chicago. In addition, many COVID-19 patients have what looks like a form of respiratory failure called ARDS, in which the lungs fare best with short, quick puffs of air from the ventilator. This feels deeply unnatural. “As humans, we like to take big breaths,” says Daniela Lamas, a pulmonary and critical-care doctor at Brigham and Women’s Hospital in Boston. All of this is so uncomfortable that doctors use powerful drugs such as propofol and fentanyl to sedate patients on ventilators. Even then, some need to have their arms and legs restrained to prevent them from ripping the breathing tube out.
When Jeri Sharp, 62, was sedated and restrained while hospitalized for ARDS from H1N1, or swine flu, in 2016, she also had frightening delusions. The proportion of intensive-care patients who experience such ICU delirium is anywhere from 20 to 87 percent, depending on the study, though it appears to be more common in patients with ventilators than in those without. Sharp remembers at one point being strapped to a bed and her legs being spread apart. “I thought I was being molested,” she says. The memory has some basis in reality: She really was restrained in bed, and a nurse was probably placing a catheter. But in her delirium, it took on a sinister cast. Other patients have reported experiencing being taken to the MRI machine as being put into an oven or misinterpreting overhead conversations as plans to kill them—then lying awake for hours trying to escape.
These delusions are experienced at the time as real, and like genuine traumatic memories, they can rewire the emotional circuits of the brain. They “can lead to PTSD just like something a person literally and really experiences can lead to PTSD,” says Shawniqua Williams Roberson, a neurologist at Vanderbilt. The drugs used in sedation alter chemicals in the brain too. These factors, Williams Roberson says, in addition to the interrupted sleep, inflammation, lack of oxygen, and toxins from kidney or liver failure that are part of critical illness, may all play a role in psychological and cognitive changes after the ICU.
Back in her moment of delirium, Sharp remembers, she was comforted by a voice she recognized—her mother saying, “Jeri, it’s okay. It’s okay.” When she woke up, Sharp learned that her mother really had been by her side for several days. COVID-19 patients in the ICU, in contrast, are no longer allowed visitors, because of the risk of infection. They are alone, and the only people they do see are strangers covered head to toe in protective gear.
The coronavirus may compound other factors in post-intensive-care syndrome too. “In the ICU, our goal is generally to keep people the least sedated as possible,” Lamas says. Research suggests that lighter sedation is linked to better outcomes. But COVID-19 patients actually need to be sedated for a long time because of the extensive damage in their lungs. They also require deeper sedation when they are turned onto their stomach, which can be uncomfortable but seems to help open up parts of the lungs to improve oxygen levels. And doctors and nurses are simply less able to check on patients when each interaction becomes an infection risk. At her hospital, Lamas says, the monitors for ventilators have been moved into the hallway so that they can be adjusted from the outside. “Which is handy,” she says. “But it also separates us from the patients quite physically and visibly. A resident said to me walking by, ‘It’s like a video game.’ And that’s true, but also a very eerie feeling of these deeply sedated humans whose faces a lot of the team has never seen.”
Patients who are able to come off the ventilator can be so weak that they cannot walk or shower on their own. They’re usually put into physical therapy right away. But it is the psychological and cognitive recovery, several patients told me, that they were never warned about when they were discharged. They fell into a gap in the health-care system. “The providers typically working in the ICU, they’re critical-care intensivists,” Jackson says. “The person who saved your life in the ICU, you can’t see them in a follow-up clinic.” Sharp told me that she once went back to the hospital to share her experience with some of the doctors and nurses who took care of her; she remembers how their eyes widened in disbelief as she spoke. They had no idea that she had been going through all that.
Today, more than three years later, Sharp says she still has trouble reading a book or adding a tip. She gets overwhelmed easily. When she started driving again, she found simply going to the grocery store to be too much. “It was too many choices to make. I got one aisle and I just started crying,” she said. “To this day, I still have trouble going to the grocery store.” She didn’t understand why she was feeling this way until she found Facebook support groups for other ARDS survivors, who experienced some of the same symptoms.
Jan Hunter, 70, told me that she had to put the pieces together herself by reading her own medical records. Beginning in late 2016, Hunter spent two and a half months in the ICU after complications from routine surgery. Once home, she continued to struggle with basic tasks and she became depressed. “I felt bad I wasn’t more grateful to be a miracle survivor,” she said. Not until later, when she started looking at her medical records, did she realize she was not alone. When she found the word delirium in her records, she learned that the hallucinations she had in the ICU were not unusual. Eventually, she learned that what she was still experiencing had a name: post-intensive-care syndrome.
Although she lives in Virginia, Hunter ended up joining a support group out of Vanderbilt in Tennessee. The group has members across the country, and they’ve been meeting every Tuesday on Zoom—long before all support groups had to go virtual in the coronavirus era.
Mullicane, who is part of the same support group, says he has been thinking about COVID-19 patients who have to be in the ICU alone. When the disease began spreading in the United States, he began pleading with his friends and family who compared it to the flu. “I’ll tell you what isn’t ‘just the flu’—it’s being on a ventilator,” he says. “I would not wish the experience on my worst enemy.” The ICU saved his life, of course, but he knows from personal experience that it changed his life too.